Tobias Franz

Tobias Franz
Former MD Student
Medical Doctor Project 6
MD6: Molecular interplay of Th2 cells and the airway epithelium on the transcriptome of alveolar type II cells during asthma
|
|
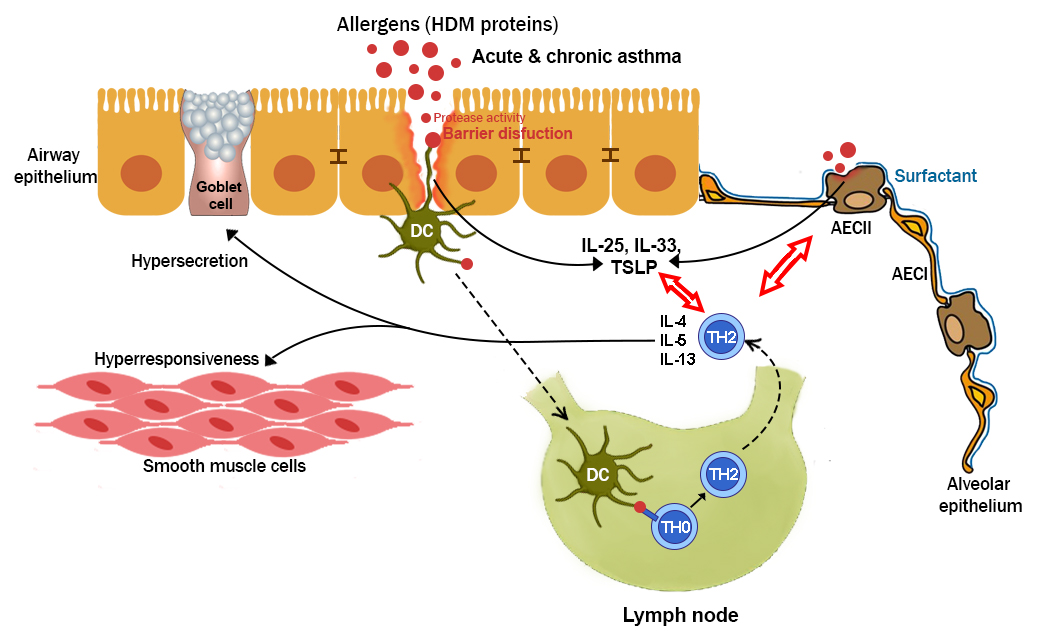
Allergic asthma is an inflammatory respiratory disease and one of the most common chronic disorders causing alterations of the airway barrier integrity. During the disease pathogenesis, allergens, e.g. from house dust mites (HDMs), evoke a maladaptation of the airway epithelia as HDM components activate receptors on airway epithelial cells (e. g. Dectin-1, TLR2, TLR4, PAR2) and destroy gap junctions between them. Consequently, airway epithelial cells produce specific cytokines including IL-25, IL-33 and thymic stromal lymphopoietin (TSLP). The latter induce an immune response that involves innate but also adaptive immune cells such as T helper (Th)2 cells. We hypothesize that Th2 cells, their metabolic fitness, and their ability to communicate with other immune cells and local structural cells in the lung may play a central role in maladaptive processes of the airway epithelia during chronic asthmatic airway inflammation. Therefore, we here will elucidate the intercellular communication of alveolar epithelial cells and Th2 cells during asthmatic airway inflammation with a special focus on analyzing the transcriptional profile of airway epithelial type II cells (AECsII) during acute and chronic asthmatic airway inflammation.
Intercellular communication between Th2 cells and airway epithelial type II cells during acute and chronic asthmatic airway inflammation. HDM proteases disrupt the airway epithelial barrier. Thereafter, HDM antigens are phagocytosed by dendritic cells (DCs) and subsequently presented in mediastinal lymph nodes to naïve T cells. HDM-primed T cells differentiate into Th2 cells, produce Th2 cytokines (IL-4, IL-5, IL-13) and migrate to the lung, where they promote a disease-amplifying micromilieu. Th2 cell cytokines mediate eosinophil recruitment, airway hyperresponsiveness, and mucus production. During the pathogenesis of allergic asthma, Th2 cells interact with airway epithelial type II cells (AECsII). How this communication affects the transcriptional fixation and maladaptation of AECsII during chronic asthma will be addressed in this project. |
Photos: by UMMD, Melitta Schubert/Sarah Kossmann