MD2: The capacity of mast cells to translate skin inflammation into systemic effects
|
|
Allergic contact dermatitis is an inflammatory skin disease that comprises 20% of occupational skin disorders. The contact hypersensitivity (CHS) is the respective mouse model, in which small organic compounds (e.g. dinitrofluorobenzene (DNFB)) are used as haptens. The hapten encounter into the skin disrupts the epidermal barrier and induces a keratinocyte stress response including the release of alarmins, e.g. IL-33 and ATP. Mast cells (MCs) sense the cell stress signals and respond by immediate degranulation of preformed mediators, such as histamine, TNF, IL-6 and IL1-β. Thereby they cause a vascular response and initiate innate immunity including the influx of neutrophils. We could recently show that perivascular MCs can pass the vascular barrier and form granule-rich intraluminal sheets. Upon inflammatory insult, these perivascular MCs degranulate directionally into the blood vessels. That is why we hypothesize that MCs are able to translate the local inflammation into systemic effects that amplify the immune response. However, this process may lead to detrimental exuberant effects. We will analyze the impact of local skin MC degranulation on I) splenic and bone marrow cell subpopulations and the recruitment of lymphoid and myeloid cells using flow cytometric analysis, II) hematopoietic niches in bone marrow by analyzing the localization of bone marrow resident cell populations using multi-epitope-ligand cartography, and III) humoral immune components, e.g. acute phase proteins, cytokines and chemokines using multiplex serum analysis. In addition to MC activation by DNFB-induced CHS, we will confirm promising findings using mastoparan, a direct MC activator. To determine the role of MCs and of MC-derived IL-6 as well as TNF we will use MC-deficient mice and mouse lines with a MC-specific gene inactivation of IL-6 and TNF.
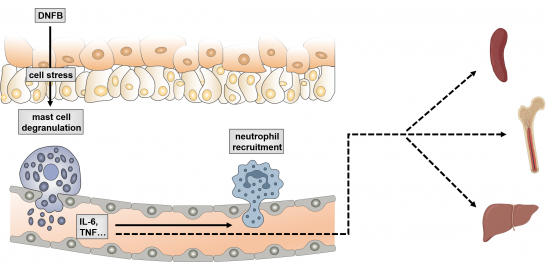
Systemic supply of TNF and IL-6 by intravascular degranulation of perivascular MCs. Epicutaneous application of DNFB leads to directional degranulation of perivascular MCs into dermal blood vessels. This induces an activation of circulating neutrophils facilitating their extravasation to the inflamed skin. We hypothesize that this MC capacity may lead to systemic effects on bone marrow, spleen and on the production of humoral components of the innate immune response. |
Photos: by UMMD, Melitta Schubert/Sarah Kossmann